Coverage for Wegovy by Blue Cross Blue Shield (BCBS) varies by individual policy and plan. Verify details with your specific BCBS provider for weight loss coverage options.
Obesity poses significant health risks and managing it is a top priority for many, prompting them to explore treatment options such as Wegovy, a prescription medication designed for chronic weight management. As individuals seek support through their healthcare plans, understanding the specifics of insurance coverage becomes essential.
Insurance providers, including various BCBS plans, may offer coverage for FDA-approved weight loss interventions; however, the extent of coverage for drugs like Wegovy often depends on your specific policy terms, formulary lists, and the necessity determined by healthcare providers. Always consult with your BCBS representative to understand the benefits and limitations of your health plan regarding weight loss medications.
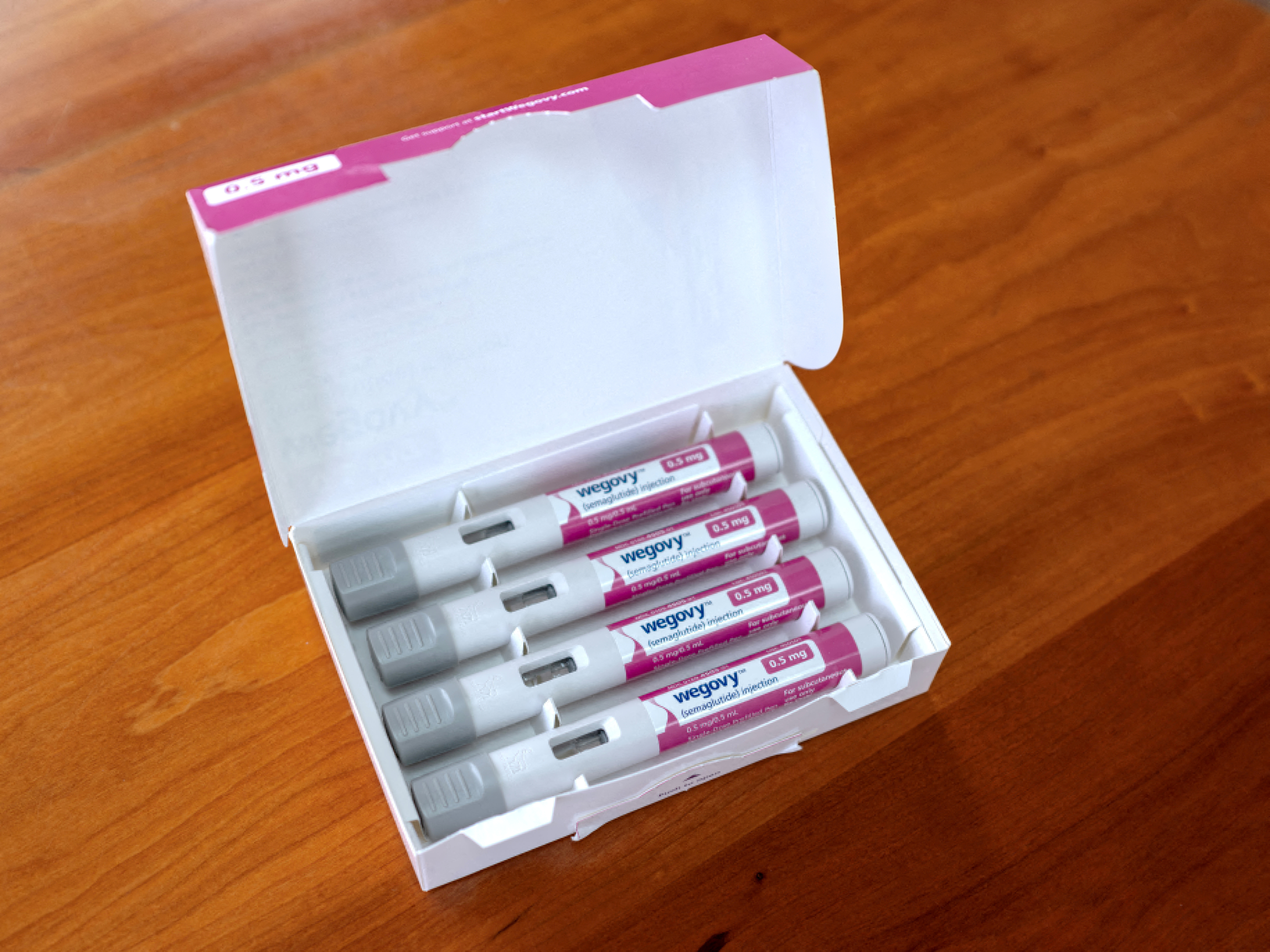
Credit: www.reuters.com Check Price in Amazon 👈
Understanding Wegovy
In the journey to manage weight, Wegovy has emerged as a notable option. This section dives into the essentials of Wegovy and explores if Blue Cross Blue Shield (BCBS) provides coverage for this weight loss medication.
What Is Wegovy?
Wegovy is a prescription medication for adults struggling with obesity or excess weight issues. It is considered when diet and exercise alone do not suffice.
How Does Wegovy Work?
It contains the active ingredient semaglutide, which mimics a hormone that targets areas of the brain involved in appetite regulation.
- Reduces hunger
- Increases feelings of fullness
Benefits Of Wegovy
The benefits of Wegovy are multifold, offering more than just weight loss:
| Benefit | Impact |
|---|---|
| Weight Management | Helps maintain a steady weight by controlling appetite. |
| Health Improvement | Supports better health markers like blood sugar levels. |
| Lifestyle Enhancement | Lends to an improved overall lifestyle and well-being. |
Coverage By Bcbs
When considering weight loss options, insurance coverage is a top concern. Many look to the Blue Cross Blue Shield Association (BCBS), known for its extensive healthcare plans, to determine if options like the new weight loss medication Wegovy are covered. This post delves into the specifics of BCBS and its coverage related to weight loss treatments.
What Does Bcbs Stand For?
BCBS represents the Blue Cross Blue Shield Association. It is a federation of 36 separate United States health insurance organizations. BCBS provides coverage for millions of Americans. BCBS offers a range of insurance plans, each with different benefits.
Does Bcbs Cover Weight Loss Treatments?
Yes, some BCBS plans do cover weight loss treatments. Coverage varies based on the specific policy and state regulations. Treatments may include lifestyle programs, surgeries, and medications.
- Lifestyle intervention programs
- Bariatric surgeries
- Prescription medications
Specifics Of Bcbs Coverage For Wegovy
BCBS coverage for Wegovy, a prescription weight loss drug, depends on the plan. Some BCBS plans may consider it a covered benefit, while others may not. Coverage can also hinge on criteria like BMI and comorbidities. Doctor recommendations play a role in determining coverage.
| Plan Type | Wegovy Coverage | Criteria |
|---|---|---|
| Standard | Potentially covered | BMI, comorbid conditions |
| Premium | Often covered | Doctor’s prescription |
To confirm coverage, policyholders should directly contact their local BCBS company. Policy documents provide detailed information regarding the coverage of weight loss medications like Wegovy.
Eligibility And Requirements
Understanding eligibility and requirements for BCBS coverage of Wegovy for weight loss is key. This medication can be a game-changer for those struggling with obesity. Let’s dive into the specifics of what it takes to qualify for coverage under BCBS plans.
Criteria For Bcbs Coverage
BCBS evaluates several criteria before approving Wegovy. Patients must meet set conditions:
- Diagnosis of obesity (BMI ≥ 30) or overweight (BMI ≥ 27) with weight-related conditions
- History of unsuccessful weight management
- Prescription by a healthcare provider
Patients should fit these criteria for potential approval.
Documentation Needed
Acquiring the necessary paperwork is crucial.
| Document | Description |
|---|---|
| Medical records | Including BMI calculations and weight history |
| Previous treatments | Details on past weight loss efforts |
| Prescription | Issued by a certified professional |
Collect these documents for the approval process.
Approval Process
Gaining approval requires a step-by-step approach:
- Submit the completed application with documentation to BCBS.
- BCBS reviews the application against their coverage policies.
- Patients usually receive a decision within a few weeks.
Follow these steps accurately for a smooth process.

Credit: www.nbcnews.com
Alternative Coverage Options
Exploring your options for covering Wegovy for weight loss is crucial. Insurance coverage can be complex. It’s important to know your alternatives. Let’s delve into the different ways you might secure coverage or manage costs for this medication.
Different Insurance Providers
Insurance benefits can vary widely between providers.
- Check with your insurer: Review your policy’s pharmacy benefits.
- Pre-authorization may be required: Your doctor might need to confirm the necessity of Wegovy.
- Compare plans: Shopping around could lead to better coverage options.
Medicare And Medicaid Coverage
Government programs might offer a path to funding this treatment.
- Medicare Part D: Check if Wegovy is on the formulary.
- Medicaid: Coverage varies by state, so inquire locally.
- Additional help: Low-Income Subsidy (LIS) might make Wegovy affordable.
Out-of-pocket Costs
Paying without insurance is sometimes necessary. Consider these strategies:
| Strategy | Description |
|---|---|
| Manufacturer’s Coupon | Use discounts offered by Wegovy’s maker. |
| Payment Plans | Some pharmacies spread payments over time. |
| Pharmacy Shopping | Prices can differ. Shop for the best deal. |
A solid grasp of your coverage options can empower your journey to better health.
Credit: www.nbcnews.com
Frequently Asked Questions For Does Bcbs Cover Wegovy For Weight Loss
Is Wegovy Covered By Bcbs For Weight Loss?
BCBS coverage for Wegovy can vary by plan and location. It’s important to check with your specific Blue Cross Blue Shield policy or through your healthcare provider to determine coverage eligibility for this weight loss medication. Pre-authorization may be required.
What Is The Cost Of Wegovy With Bcbs Insurance?
The cost of Wegovy with BCBS will depend on your insurance plan’s structure, including deductibles, copayments, and coinsurance. Your local BCBS can provide exact pricing based on your current benefits. Sometimes, manufacturer discounts or patient assistance programs may be available.
How To Get Bcbs Approval For Wegovy Treatment?
To obtain BCBS approval for Wegovy, your doctor must submit a prior authorization request detailing the medical necessity for your weight loss treatment. Your plan may require documented evidence of previous weight loss efforts before granting approval.
Can I Appeal If Bcbs Denies Wegovy Coverage?
Yes, you can appeal BCBS’s decision if they deny coverage for Wegovy. The process typically involves submitting a formal appeal letter with additional information and support from your doctor. BCBS will review the appeal before making a final decision.
Conclusion
Navigating the specifics of insurance coverage can be daunting, particularly for a drug like Wegovy. It’s essential to consult with Blue Cross Blue Shield directly to determine your policy’s stance on obesity treatment. Armed with the right information, you’ll be better prepared to explore Wegovy as a potential ally in your weight loss journey.
Remember, individual plans may vary.


Wow Thanks for this posting i find it hard to identify extremely good resources out there when it comes to this topic thank for the thread website
Wow Thanks for this publish i find it hard to come across excellent specifics out there when it comes to this material thank for the information site
Wow Thanks for this content i find it hard to uncover smart resources out there when it comes to this subject matter thank for the article website
nice blog mate.. amazing content.. this one i search for. thank you
Wow Thanks for this post i find it hard to acquire decent ideas out there when it comes to this blog posts thank for the review site
Wow Thanks for this posting i find it hard to get a hold of great advice out there when it comes to this subject material appreciate for the guide site
Wow Thanks for this article i find it hard to discover awesome specifics out there when it comes to this topic appreciate for the write-up site
Wow Thanks for this article i find it hard to search for very good facts out there when it comes to this material thank for the thread site
Wow Thanks for this article i find it hard to stumble on really good information out there when it comes to this blog posts thank for the guide site
Wow Thanks for this thread i find it hard to see excellent important information out there when it comes to this material appreciate for the write-up site
Thanks!